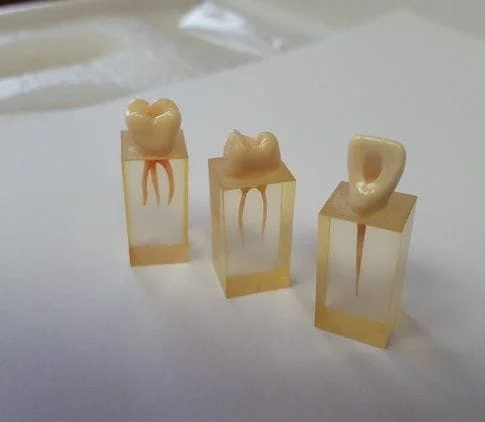
Endodontics is the dental specialty that deals with the pulp ("nerves") of the teeth. The pulp is the soft tissue in the center of the tooth responsible for tooth sensitivity, hydration of the tooth itself, and defense against invaders such as bacteria. When the pulp sustains injury, whether it be from trauma or an irritant such as a cavity or a very deep filling, it can become inflamed and may even lead to cell death (necrosis). When this happens, an infection develops. If left untreated, an infection can turn into an abscess, which is a much more serious problem that includes bone loss in the jaw and possible life-threatening systemic involvement.
In cases when the pulp becomes inflamed irreversibly or when the pulp dies, the only solutions are root canal therapy (meaning the removal of the infected pulpal tissues) or extraction of the entire tooth.
To accomplish root canal therapy, the area around the tooth is numbed with a local anesthetic to start the procedure. We then drill down into the tooth to create an opening into the canal system inside the root. We will then be able to remove the infected or inflamed tissue and clean the canal. After the infection has been removed, the space is filled with a sealant called gutta percha. Since root canal treated teeth are prone to fracture, it is highly recommended in most instances that the tooth be fitted for a crown.
"Root canal" has become a scary term for dental patients to hear, but the benefits of the procedure and advances in dental technology have made it much less "scary." Local anesthetics and proper pain medication allow the procedure to be performed with little to no pain in most cases.
If you need post-operative instructions for how to care for your mouth after a root canal treatment, you can find them on this website under Patient Resources and then under Post-Op Instructions.